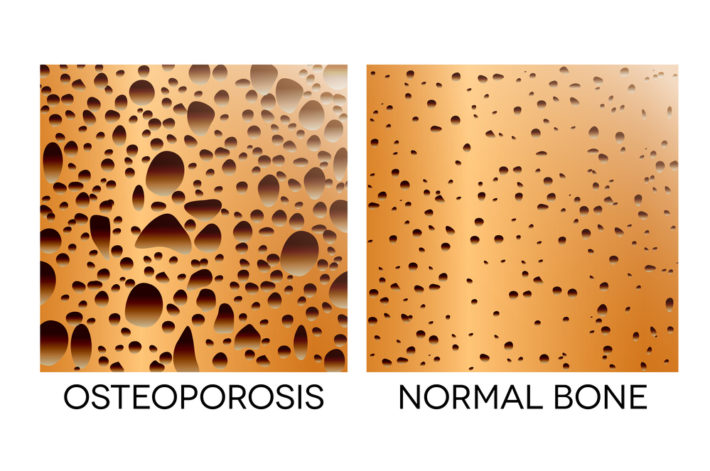
Bone health!
Boring, right!?
Better to worry about breast health; getting a mammogram and making sure you don’t have breast cancer.
Well, that is really important.
But as I tell my Menopause Coaching clients, if you are a healthy fifty year old woman, your just as likely to die from a complication of osteoporosis as your are from breast cancer.
There is one major difference. Breast cancer is diagnosed AFTER it happens. Osteoporosis can be diagnosed BEFORE it happens.
Here are Nine Facts you should understand to protect your bones according to the North American Menopause Society (NAMS):
- Osteoporosis is a common disorder with potentially serious consequences. Over 300,000 people break their hip each year
- Testing your bone health should be a part of routine care for all postmenopausal women. I recommend getting a baseline bone density at 50 years, or at 40 if there is a history of a broken bone or a family history of osteoporosis.
- The annual examination should include measurements of height and weight; assessment for chronic back pain and kyphosis; and clinical risk factors for osteoporosis, fractures, and falls – things like old glasses prescriptions, rugs that aren’t even, no night light to see going to the bathroom, and others.
- The most important risk factors for future fracture are a history of previous fracture, older age, and low bone mineral density (BMD). – Fracture risk is especially high in the first 2 years after a significant loss of bone on a scan or loss of height.
- Bone mineral density testing is indicated for all postmenopausal women with risk factors for low BMD or fracture. – DXA (sounds like Dexa and stands for “dual-energy X-ray absorptiometry”) is the preferred technique for BMD testing. – For untreated postmenopausal women at low fracture risk, repeat DXA testing is not useful until at least 5 years have passed, unless rapid bone loss is anticipated. People who do have risk factors should have a DEXA every other year.
- Vertebral imaging is appropriate for postmenopausal women aged 70 years and older or with historical height loss.
- Be sure that any bone loss is due to natural loss and not some other reason such as a medical condition that takes calcium out of the bones. Once that is done, osteoporosis treatment should be started.
- The routine use of biochemical markers of bone turnover, ie blood or urine tests that say you are losing bone too rapidly, in clinical practice is not recommended.
- Estrogen, if started near the start of menopause, is an excellent way to help prevent osteoporosis. Taking calcium, vitamin D3, and magnesium are also helpful.
If you are getting shorter, it may be because calcium is coming out of your spine. That is a good reason to talk with your doctor about diagnosing and preventing further bone loss.