Most people don’t think about their bones much until they break or ache. Unlike our teeth, our bones are buried beneath our skin, muscles, and fat. Like so many other parts of a woman’s body, bones have a close relationship with estrogen and have an estrogen window.
The bones are where the body stores most of its calcium. As girls develop into young women, they incorporate literally pounds of calcium into their bones to help them grow. The majority of the body’s growth is complete and bone density is at its highest by the time a young woman reaches her late teens and early twenties. Medically speaking, bone density refers to the amount of mineral matter per square centimeter of bone. Calcium and magnesium are most essential for bone growth, but vitamins C, D, and K and small amounts of trace minerals, such as copper and zinc, also play important roles. Calcium is necessary for body functions such as muscle and nerve function, blood clotting, and others.
Bone is living tissue. Bone tissue constantly breaks down and rebuilds and repairs itself. Compact bone is the strong, hard outside part of the bone that makes up most of the human skeleton. Cancellous bone is the spongy tissue inside compact bone where red and white blood cells are formed in the marrow.
Calcium is about 1.5 to 2 percent of our body weight. About 98 percent of the approximately 3 pounds of the calcium in our body is in our bones, about 1 percent is in our teeth, and the final 1 percent is in other tissues and in our circulation at a concentration of about 10 mg/mL. When calcium beyond what is taken in from our diet is called on to carry out certain functions, parathyroid hormone increases. This leaches calcium out of the bones, and increases absorption from our intestines, so our bones must absorb more calcium to maintain its effectiveness and to prevent weakening of the bones.
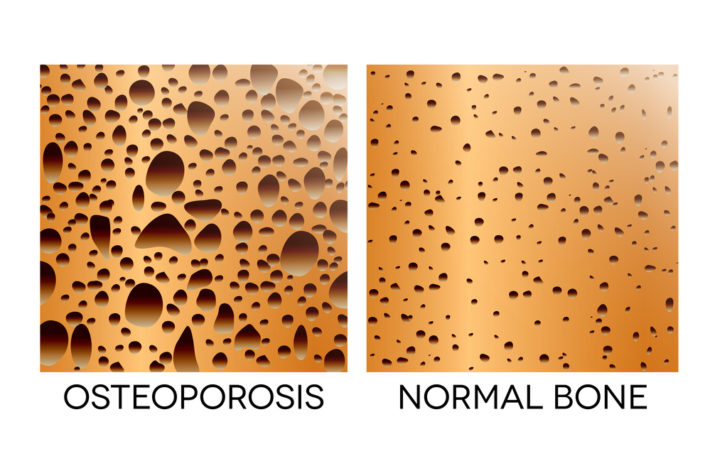
Failure to adequately absorb calcium is one cause of bone loss from osteopenia (when bones are not as strong as they should be because of loss of calcium) and osteoporosis (when bones are so weak, they easily fracture). At their simplest level, bones are constantly in a state of remodeling, which is the term used to describe their natural breakdown and repair process. Osteoblast cells build bone; osteoclast cells break bone down. During the years of growth and higher estrogen levels in women, there is more osteoblast activity than osteoclast activity. During most of a woman’s adult years, these two cell types stay in balance. In menopause, because estrogen does suppress osteoclasts somewhat, the roles are reversed, and osteoclast activity becomes greater than osteoblast activity as estrogen levels decline. It’s also important to mention the role of testosterone, which stimulates osteoblasts. For women who have had a hysterectomy and who are taking estrogen and still losing bone density, adding testosterone can help. Estrogen slows the osteoclasts’ breakdown of bone; testosterone increases the action of osteoblasts to build more bone.
The bones contain estrogen receptors, particularly the alpha receptors, which allow estrogen to stimulate them. Estrogen increases the activity and number of osteoblast cells. These cells place calcium into bones to fill in cracks and hairline breaks and help bones grow and stay strong. Lack of estrogen causes more bone to be broken down and removed as calcium enters the bloodstream to participate in the physiology of the body. In essence, the bones are the calcium savings account of the body. The more calcium you store in your bones earlier in life by maintaining a diet rich in calcium, exercising regularly, and not smoking, the stronger your bones and the greater your “calcium savings account” will be as you age.
As women enter perimenopause, menopause, and beyond and estrogen levels become lower, their bones also enter their estrogen window. The estrogen receptors on bone cells that allow estrogen to exert its actions start to decline, and the activity of osteoclasts increases. With lower levels of estrogen, inflammatory cytokines increase (just like they do in the blood vessels) and contribute to faster bone loss. These bone-losing processes that occur naturally with lower estrogen can be reversed with estrogen or with SERMs (selective estrogen receptor modulators) that work by selectively stimulating the estrogen receptors on bones.
Without question, science has established that estrogen is crucial for bone health in women and is an estrogen fix. When estrogen production is reduced in postmenopausal women, their bones slowly develop osteopenia and osteoporosis and become brittle and break more easily. Even in the 2002 WHI study and many others that have followed, ET (estrogen only therapy) and EPT (estrogen and progestin therapy) have been shown to lower the risk of osteoporosis.
And as is true with most other tissues, there is an estrogen window. Early interventions pay great dividends. Research done by Dr. Robert Lindsay helped to fine-tune the estrogen window for bone. When the ovaries were removed, causing surgical menopause, and estrogen was replaced immediately, there was no bone loss over the next 12 years. If after removal of both ovaries there was a delay of 3 years before beginning estrogen, those women lost 10 percent of their bone density. But if estrogen was given at that time, the bones were able to regain the lost density. If 6 years passed after removal of both ovaries before estrogen was taken, there was no additional bone loss, but the bones were also unable to regain any of their lost density. So the estrogen window for bones appears to be about 6 years, but it is most effective if estrogen is begun as early as possible after surgical menopause.

Would you like to better understand how and when to take estrogen, how lo estrogen effects the other organs of your body, or even what to do if you can’t take estrogen, get your copy of The Estrogen Fix. If you buy it before September 19, you’ll also get some great free gifts as a thank you for supporting this important information for women’s health. This book has been recommended by the North American Menopause Society (NAMS) not only for women but also for the doctors who take care of them.
“In his new book, The Estrogen Fix, Mache Seibel, MD, has created a breakthrough guide to coach women through menopause. He clarifies how to manage menopause symptoms, balance the risks and benefits of hormone therapy and when might be the best time to consider treatment, and how to communicate effectively with your doctor. Highly recommended for anyone dealing with menopause issues.”
–Steven Masley, MD, FAHA, FACN, FAAFP, CNS, bestselling author of Smart Fat and The 30-Day Heart Tune-Up and creator of top public television programs: 30 Days to a Younger Heart and Smart Fats to Outsmart Aging.